The IT Innovator’s Guide to Digital Transformation in Health Care

INTRODUCTION: THE NEW ERA OF HEALTH CARE
Healthcare technology is one of the fastest growing IT markets today, with estimates reaching $280.25 billion by 2021 from $134.25 billion in 2016.[1] Technologies such as electronic health records, patient managing systems and even pill dispensing systems are contributing to this growth; in fact, the clinical solutions segment within healthcare IT is poised to grow almost 13 percent CAGR between 2017 and 2022.[2]
The growth of healthcare-related technology now enables health providers to provide levels of service previously unheard of. Moving well beyond the traditional reactive approach to treating patients, doctors and other healthcare workers are using technology to predict health trends among populations and moving proactively to address issues before they occur.

Advancements in technology carry implications that reach well beyond improvement of patient care, however. Back office operations also are realizing the benefits of services enhanced by technology. And, in a domino-like effect, those enhancements are, in turn, impacting everything from the way healthcare facilities share information to the models by which they are compensated for their services.
Healthcare technology is reliant on a solid network that can easily handle the bandwidth needs of different systems within a facility and beyond. It is imperative that healthcare facilities have a network that is powerful enough to support an infrastructure capable of supporting the technologies enhancing patient care and those improving back office operations.
THE CHANGING HEALTHCARE BUSINESS LANDSCAPE
Technology’s impact on health care has proven itself multiple times as a catalyst to more impactful patient/provider relationships, enhanced patient care and improved provider operations. It also has spurred government agencies and other entities to enact policies that reward or penalize providers based on their use or non-use of specific technologies, such as electronic health records (EHRs).
The Centers for Medicare and Medicaid Services (CMS), for example, provides financial incentives to healthcare professionals and facilities for their use of EHR. Meaningful Use, which took effect in 2011, pays providers as much as $63,750 and hospitals as much as $6 million for using EHR that, as a result, increases patient and family and patient engagement and ultimately leads to improved outcomes. Those that don’t comply with Meaningful Use, however, receive less compensation for patient care from Medicare.
Beyond that, CMS has initiated the Value-Based Payment Modifier Program, which provides payment for services to physicians based on annual cost and quality measures, and the Hospital Readmission Reductions Program (HRRP), which penalizes hospitals that have relatively higher rates of Medicare readmissions. According to KFF.org, Medicare penalties assessed on hospitals for readmissions will total $528 million in 2017, an increase of $108 million from 2016.[3]

These value-based care models rely on data, not only for providers and agencies to determine payments, but also for providers to assess their performance and target potential areas of improvement. To achieve that, healthcare providers need to measure and analyze patient data continuously.
Apart from determining payments, healthcare providers can use collected patient data in population health initiatives, a trend that has taken hold within the healthcare sector to be proactive in preventing disease and promoting health through outreach and education. The need for population health initiatives is real: A study by the Commonwealth Fund revealed the United States spends far more on health care per patient than other countries, yet its citizens have a shorter average life expectancy.[4]
Healthcare providers can take advantage of collected patient data to target populations that can benefit from population health initiatives, such as communities with high instances of Type 2 diabetes or chronic obstructive pulmonary disease, for example.
Population health initiatives are helping pave the way for medical groups and health systems of hospitals at a more micro level, demonstrating an impact that can be felt across neighborhoods or local demographics. One group of healthcare facilities in Illinois, for example, was able to use big data and predictive analytics to target patients who had the highest risk of hospital readmission and take steps to mitigate the risk before they were discharged.[5]
The benefits of population health initiatives are numerous. Not only do they help improve overall patient health through active management of existing conditions and preventative care to head off potential health issues, they ultimately reduce the cost of health care through more targeted and streamlined treatment. A growing number of healthcare facilities understand the benefits—85 percent of hospitals taking part in one study reported a strong or total commitment to population health.[6]
TECHNOLOGIES DRIVING THE NEW HEALTHCARE ECOSYSTEM
The advent of technologies that facilitate improved patient care such as EHRs, Internet of Things (IoT), big data and analytics and even wearable technology is having a profound impact on the way providers and patients alike are approaching and consuming health care. Each technology provides more—and more insightful—patient information and enables a deeper understanding of medical trends on a micro and macro level, helping healthcare practitioners better diagnose and treat conditions among individuals and populations. Ultimately, that can lead to a shift to a more proactive rather than reactive healthcare experience.
Electronic Health Records
EHRs, for instance, are changing the face of patient record- keeping, replacing large, bulky, paper-based patient files with computer-based files accessible to authorized people simply by logging on to the office’s network and enabling instant access anytime, anywhere. EHRs have proven themselves essential in helping providers better diagnose and treat patients by having comprehensive patient medical records available at their fingertips.
Healthcare providers and facilities using electronic health records are now reaping benefits in the form of more accurate diagnoses and fewer patient visits, resulting in higher patient satisfaction rates. Because patient information is added to the EHR at the point of care, records are consistently up to date and accessible to all the patient’s healthcare providers, who can use the information to provide more holistic health care.
Internet of Things, Big Data and Analytics
Of all technologies in the healthcare space, IoT holds the greatest promise in terms of overall quality of service, accuracy in diagnosing and treating illnesses, and efficiency of healthcare operations in both time and money. IoT can help caregivers pinpoint and diagnose ailments through data analytics, help nurses and other healthcare workers provide higher-quality patient care in hospitals through smart devices and help researchers identify outbreaks of viruses or contagious illnesses through data mining and parsing of patient records.
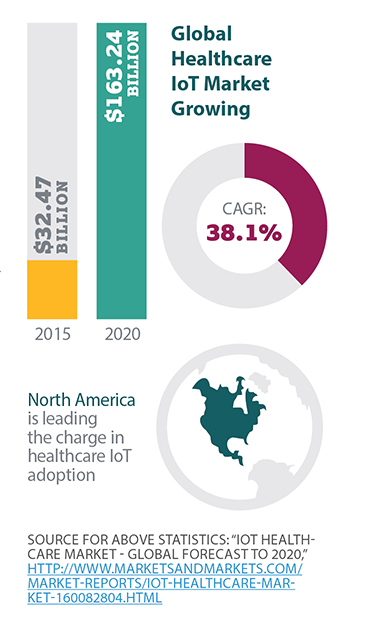
The global healthcare IoT market is expected to grow $163.24 billion by 2020, from $32.47 billion in 2015, a CAGR of 38.1 percent, with North America expected to lead the charge.[7] That number includes the myriad devices, software and systems necessary to run IoT, as well as the connectivity, services and applications.
IoT can serve a number of roles in clinical settings, from collecting valuable patient vital signs via wearable devices to enabling systems to communicate to assist in diagnoses and treatments. IoT’s value relies on big data analytics to process the myriad data collected and send out actions based on the data, giving healthcare providers the critical information necessary to provide accurate care faster and more efficiently.
Wearables
The healthcare community increasingly is relying on wearable technologies to help monitor patients’ day-to-day health and better diagnose and treat illnesses and chronic conditions.
Wearable devices can be used to monitor and manage health issues ranging from the mild (such a measuring a person’s stride to diagnose foot problems) to the critical (such as monitoring a person’s heart rate to catch any signs of failure).
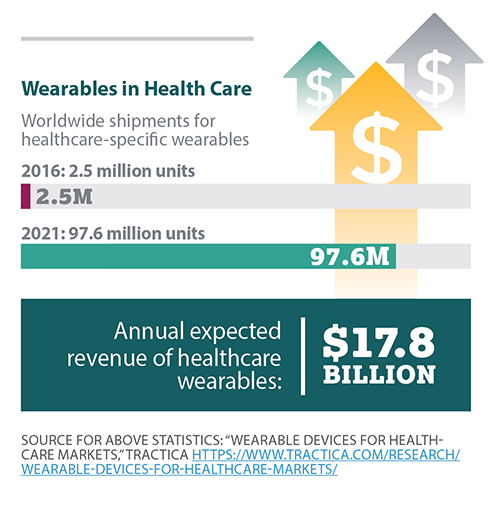
Wearables have the power to transform health care as we know it, enabling physicians and other caregivers to better manage illness and chronic conditions and even work proactively to prevent health issues before they occur. Market intelligence firm Tractica sees worldwide shipments for healthcare-specific wearables numbering 97.6 million units by 2021, from 2.5 million units in 2016, and worth $17.8 billion in annual revenue.[8] The healthcare wearables market is comprised of more than fitness bands. Smart watches, smart glasses, smart footwear, smart apparel, posture monitors, movement sensors, wrist devices, heart straps, headbands, wearable patches, pain management devices and medicine delivery pods are some of the myriad devices that make up the vast and growing healthcare wearables market.
NETWORKS CONNECT THE DISTRIBUTED ECOSYSTEM
Today’s healthcare ecosystem is much broader than the single-office patient visits of yesterday, which have largely been usurped by medical groups and affiliated facilities that can treat all manner of health conditions. As such, patients now expect that healthcare facilities and providers already have the information they need to treat them no matter what location they visit. Healthcare providers, then, must focus on providing a consistent experience across all locations.
The efficiencies afforded by machine-to-machine interaction offer healthcare facilities efficiencies not previously available. For example, an EHR system can automatically ready a patient’s healthcare record upon check-in to the doctor’s office or other healthcare facility. Or, it can notify a patient’s insurance company of necessary treatments automatically and then bill the insurance company once the treatment has been performed. Such machine-based interactions free healthcare workers to focus more on offering quality patient care and less on time-consuming back-office functions. What’s more, they eliminate the possibility of humans introducing billing code errors, which often result in longer reimbursement cycles and frustration for both the physician and the patient.
In addition, making patient information available for blind studies, research or population health initiatives requires facilities and providers can not only collect required information in a timely manner, but also deliver it to its intended recipient quickly and securely.
What’s more, the technologies used to comply with government mandates such as Meaningful Use or the Value-Based Payment Modifier Program must connect with the right systems for data collection and reporting.
Dedicated, broadband and WiFi connections are necessary to support the technologies necessary for high-quality operational experiences and improved patient outcomes.
HAVING THE RIGHT NETWORK
To ensure always-on connectivity today and provide the path for advanced technologies down the road, healthcare providers should look for a network service provider that can provide a secure, high-performance network that can be adjusted to meet dynamic bandwidth needs. A good network service provider will address current demands and anticipate future needs of healthcare facilities to ensure patient care remains top-notch and customer-focused.
Look for a network provider who can handle every aspect of the network, from provisioning to management and field technology services, for installation, maintenance and repairs. That way, healthcare providers can focus on providing the best experience possible instead of tending to their networks.
[1] RESEARCH REPORT, “HEALTHCARE IT MARKET BY PRODUCT (EHR, RIS, PACS, VNA, CPOE, HIE, TELEHEALTH, HEALTHCARE ANALYTICS, POPULATION HEALTH MANAGEMENT, SUPPLY CHAIN MANAGEMENT, CRM, FRAUD MANAGEMENT, CLAIMS MANAGEMENT) END USER (PROVIDER, PAYER) - GLOBAL FORECAST TO 2021,” MARKETS AND MARKETS, MARCH 2017, HTTP://WWW.MARKETSANDMARKETS.COM/MARKET-REPORTS/HEALTHCARE-IT-252.HTML
[2] RESEARCH REPORT, “ECLINICAL SOLUTIONS MARKET BY PRODUCT (CDMS, EDC, CTMS, ECOA, ANALYTICS, RTMS, ETMF, SAFETY), DELIVERY MODE (ON-DEMAND, ON-PREMISE, CLOUD-BASED), CLINICAL TRIAL PHASES, END USER (PHARMA/BIOPHARMA COMPANIES, CROS, HOSPITALS) - GLOBAL FORECAST TO 2022,” MARKETS AND MARKETS, APRIL 2017, HTTP://WWW.MARKETSANDMARKETS.COM/MARKET-REPORTS/ECLINICAL-SOLUTIONS-MARKET-553.HTML
[3] AIMING FOR FEWER HOSPITAL U-TURNS: THE MEDICARE HOSPITAL READMISSION REDUCTION PROGRAM,” ISSUE BRIEF, KFF.ORG, SEPT. 30, 2016, HTTP://KFF.ORG/MEDICARE/ISSUE-BRIEF/AIMING-FOR-FEWER-HOSPITAL-U-TURNS-THE-MEDICARE-HOSPITAL-READMISSION-REDUCTION-PROGRAM/
[4] U.S. HEALTH CARE FROM A GLOBAL PERSPECTIVE,” REPORT, THE COMMONWEALTH FUND, OCT. 8, 2015, HTTP://WWW.COMMONWEALTHFUND.ORG/PUBLICATIONS/ISSUE-BRIEFS/2015/OCT/USHEALTH-CARE-FROM-A-GLOBAL-PERSPECTIVE
[5] MUCH MORE THAN JUST A NUMBER: HOW DATA ANALYTICS, THE CLOUD AND HIGH-CAPACITY NETWORKS ARE IMPROVING POPULATION HEALTH,” WHITE PAPER, COMCAST/HIMSS MEDIA, 2016
[6] APPROACHES TO POPULATION HEALTH IN 2015: A NATIONAL SURVEY OF HOSPITALS,” STUDY, AMERICAN HOSPITAL ASSOCIATION, AUGUST 2015 HTTP://WWW.HPOE.ORG/REPORTS-HPOE/201/POPHEALTHSURVEY_FINAL_PICTURE.PDF
[7] RESEARCH REPORT, “IOT HEALTHCARE MARKET - GLOBAL FORECAST TO 2020,” OCTOBER 2015, HTTP://WWW.MARKETSANDMARKETS.COM/MARKET-REPORTS/IOT-HEALTHCARE-MARKET-160082804.HTML
[8] WEARABLE DEVICES FOR HEALTHCARE MARKETS,” TRACTICA, APRIL 15, 2016 HTTPS://WWW.TRACTICA.COM/RESEARCH/WEARABLE-DEVICES-FOR-HEALTHCARE-MARKETS/
To ensure always-on connectivity, healthcare providers require a secure, high-performance network that can be adjusted to meet dynamic bandwidth needs.
Locked Content
Click on the button below to get access
Unlock NowOr sign in to access all content on Comcast Business Community
Resource Center
Learn how Comcast Business can help
keep you ready for what's next.











